In this previously recorded Live Demo, we will show you how our Claims Harvesting and Employer Invoicing products for Benefits TPAs streamline work processes, enabling our clients to grow accounts while winning new business.
Minimize the time and resources spent managing claims and generating invoices. Give your clients a higher level of service with speedier processing and accurate information. Let us show you how using our platform makes your job easier.
Tools for TPAs
Claims Harvesting
Securely collect EOBs from insurance carriers and access then in a web app for easy processing. Easily view EOB details and manage claim reimbursements. Using this tool helps customers get reimbursed quickly with accurate payments.
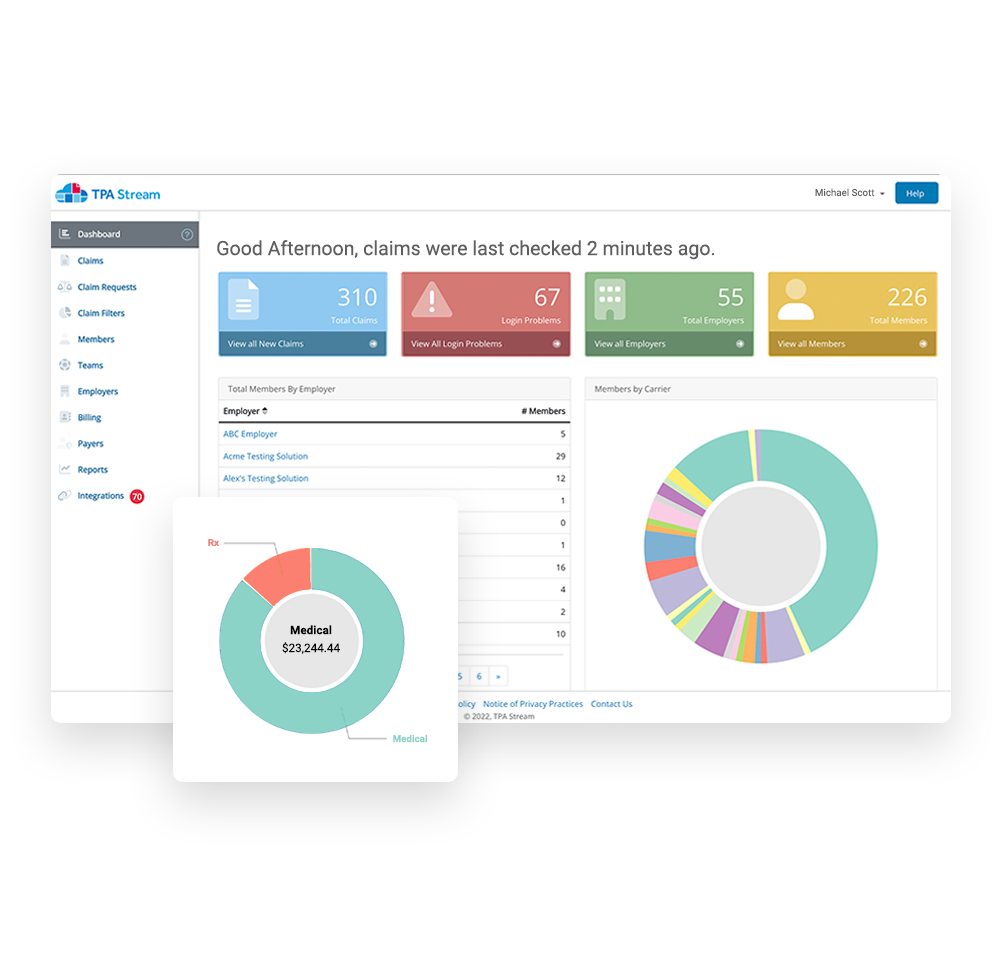
Employer Invoicing
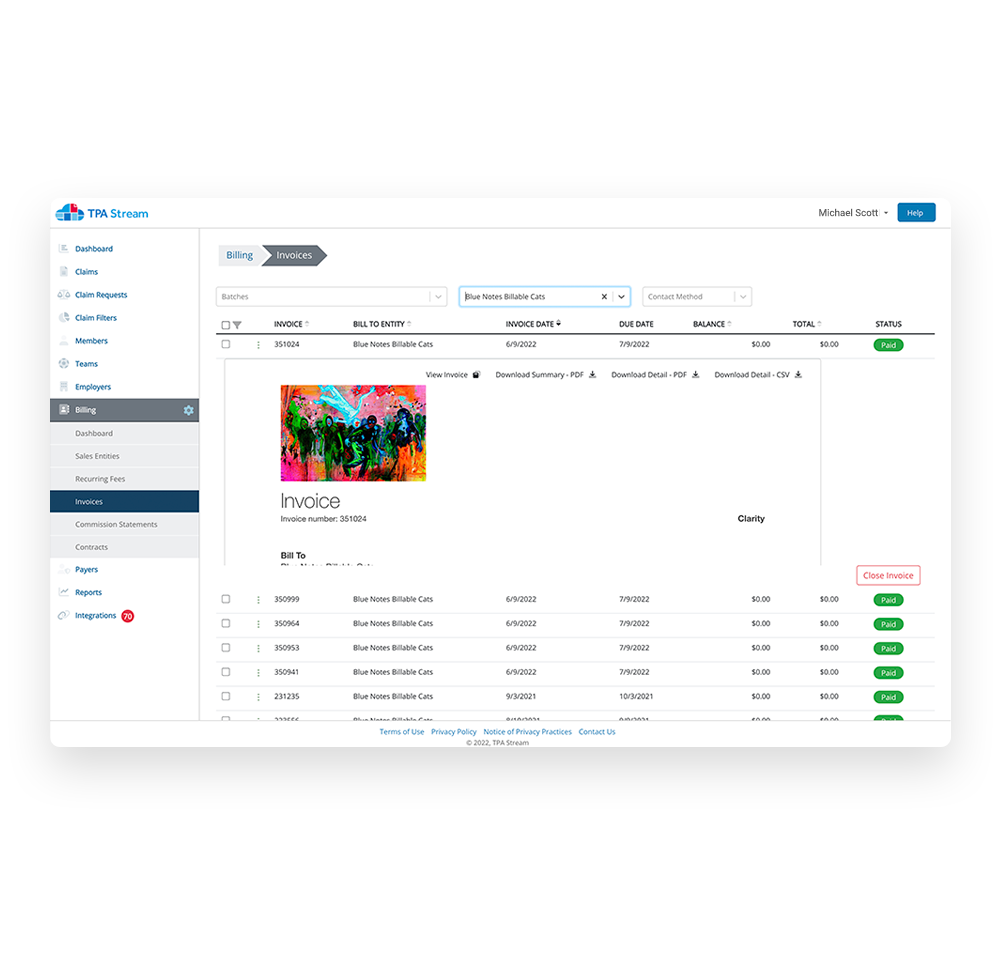
Manage sales records, invoices, recurring fees, and commission reports with one automated process. Create and customize invoices to suit whatever needs you or your clients have. Our clients distribute and track invoices online within minutes, enabling them to get paid faster.
What our customers say
Learn why TPAs love our solutions
"We were looking for more than a provider — we were looking for a partner, and we found that partner in TPA Stream. Clarity has been growing by 40 percent over the past three years. TPA Stream has definitely been part of that growth." Bill Catuzzi, CEO | Clarity Benefit Solutions
"We have clients who want things very customized for them in every way across the board, and invoicing is no different. We can now produce 30 different ways of invoicing without creating 30 different processes. It’s a 30 minute process to produce 30 different things, whereas before that it would’ve been a 5 day long thing." Mary Catherine Tompkins, VP Finance | Admin America
"In the past, my team had to spend so much time generating invoices and getting them out in a timely manner. We’re now focused more on the accounts receivable side, following up with clients and getting money back to OCA faster." Ross Honig, President | OCA
How does it work?
Claims Harvesting
Employer Invoicing
About Us
At TPA Stream, we've always focused on making benefits easier for everyone. We enable administrators, health insurance brokers, and application developers to deliver best-in-class solutions for their clients. To date, we've transformed the benefits experience for over 3 million employees - and we're just getting started.
